Does birth control prevent endometrial cancer? Discover evidence-based answers from Dr. Lucas Minig (Valencia, Spain). Learn which methods lower risk, fertility tips.
Introduction
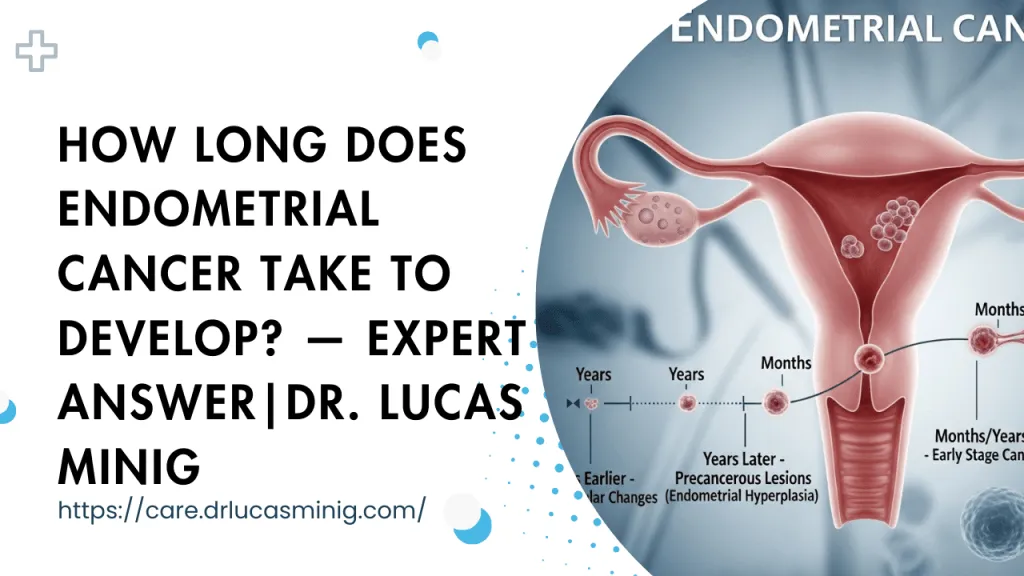
Endometrial cancer—the cancer of the uterine lining—is a significant concern for many women because its earliest symptoms are often subtle and because hormonal factors play a central role in its development. Understanding preventive strategies, including the role of birth control, helps women and clinicians make informed choices that balance contraception, symptom control and long-term cancer risk reduction.
In clinical practice across Spain, gynecologists routinely discuss contraception not only for family planning but also for its broader effects on uterine health. Dr. Lucas Minig and his team incorporate this preventative perspective into consultations, offering both medical and surgical options tailored to each patient’s reproductive goals and risk profile.
What Is Birth Control?
Birth control is any method used to prevent pregnancy. Methods range from barrier devices and copper IUDs to hormonal options (pills, patches, implants, injections, and hormonal IUDs) that change ovarian function or the uterine lining to stop conception.
Hormonal vs non-hormonal birth control
Hormonal methods deliver synthetic hormones (estrogen, progestin, or both) to suppress ovulation, thicken cervical mucus, and thin the endometrium. Non-hormonal methods, like the copper IUD or condoms, prevent pregnancy by physical or chemical means without changing the hormonal balance.
Common birth control methods used in Spain
In Spain, clinicians and patients commonly choose:
- Combined oral contraceptive pills (COCs) — widely prescribed for contraception and cycle control.
- Levonorgestrel-releasing IUDs (LNG-IUS, e.g., Mirena) — popular for long-acting contraception and heavy-period management.
- Progestin-only pills and implants — chosen for breastfeeding women or when estrogen is contraindicated.
- Copper IUDs and barrier methods — non-hormonal options used by many.
Spanish gynecologists routinely counsel patients about both contraceptive effectiveness and non-contraceptive benefits (such as menstrual control or reduced endometrial cancer risk).
Does Birth Control Prevent Endometrial Cancer?
Many large studies show a clear association: hormonal birth control that includes progestin lowers the risk of endometrial (uterine) cancer. This benefit is most consistent with combined oral contraceptives and levonorgestrel IUDs.
Quick explanation
Progestin opposes estrogen’s stimulating effect on the endometrium, reducing the chance that endometrial cells will undergo the abnormal growth that becomes cancer. Public-health analyses estimate meaningful reductions in endometrial cancer incidence among long-term hormonal contraceptive users.

How Hormonal Birth Control Protects the Endometrium?
Hormonal contraception changes the hormonal environment of the uterus and ovaries. By lowering endometrial proliferation and sometimes causing endometrial atrophy, progestin-containing methods reduce the substrate where cancer can develop.
Estrogen dominance explained simply
When the endometrium is exposed to estrogen without enough progesterone (unopposed estrogen), it keeps growing and shedding irregularly. Over years, that persistent stimulation increases the chance of DNA mistakes and abnormal cells.
How progestin counteracts cancer risk?
Progestin (the ‘P’ in many contraceptives) makes the endometrium thinner, less proliferative, and more stable. This biological effect lowers the probability of pre-cancerous changes and therefore reduces long-term cancer risk.
Which Types of Birth Control Lower Endometrial Cancer Risk?
Not all methods affect endometrial cancer risk equally. The strongest evidence and clinical rationale favor options that expose the endometrium to progestin.
Combined oral contraceptive pills
Combined pills (estrogen + progestin) are the best studied. The more years a woman uses them, the greater the protective effect against endometrial cancer. Protection also persists for many years after stopping the pill.
Progestin-only pills
Progestin-only pills likely confer protection by the same mechanism (endometrial opposition to estrogen), though large-scale data are less abundant compared with combined pills.
Hormonal IUDs (Levonorgestrel IUD)
The LNG-IUS delivers levonorgestrel locally to the uterus, causing pronounced endometrial thinning. It is used both as a contraceptive and therapeutically for endometrial hyperplasia, and studies report lower endometrial cancer incidence among users.
Injectable and implant contraceptives
Long-acting progestin injectables and subdermal implants also expose the endometrium to progestin and are expected to reduce risk; evidence supports benefit though sample sizes vary.
How Strong Is the Protection? What Studies Show?
Overall, the evidence is consistent and robust: hormonal contraception reduces endometrial cancer risk, with magnitude varying by method and duration.
Risk reduction percentages explained simply
- Each 5 years of oral contraceptive use typically cuts endometrial cancer risk by roughly 20–25%.
- Lifetime or long-term use is often associated with a 30–50% lower risk compared with never-users.
- LNG-IUS users in recent registries show risk reductions around 30% in some analyses.
These are relative reductions — absolute benefit depends on baseline risk (age, weight, PCOS, family history).
How long protection lasts after stopping birth control?
Protection does not vanish immediately. Epidemiological studies show that reduced risk can persist for decades after discontinuation of oral contraceptives, meaning past use still contributes to lower lifetime risk.

Who Benefits the Most From Birth Control’s Protective Effect?
Certain groups gain a greater absolute benefit because their baseline risk of endometrial cancer is higher.
Women with PCOS
PCOS commonly causes irregular ovulation and prolonged unopposed estrogen exposure. Using hormonal contraception (especially with progestin) helps regulate cycles and lowers endometrial cancer risk — a major consideration in management.
Women with obesity or irregular cycles
Obesity increases estrogen production from fat tissue, heightening endometrial stimulation. For women with obesity or chronic irregular cycles, progestin-containing contraception provides measurable protective value.
Women with family history of uterine cancer
A family history may raise clinical vigilance. While hormonal contraception can lower risk, genetic risk often requires tailored surveillance and genetic counseling when hereditary syndromes are suspected.
Birth Control Use in Spain: Dr. Lucas’ Perspective
In many Spanish clinics, gynecologists combine prevention and personalized care: contraception is not only pregnancy prevention but part of long-term health planning. Dr. Lucas, a gynecologist working with patients across Spain, emphasizes individualized counseling — discussing cancer-risk reduction alongside side effects, fertility plans, and lifestyle advice.
How gynecologists in Spain approach prevention?
Spanish gynecologists often:
- Review personal risk factors (BMI, PCOS, family history).
- Discuss contraceptive options that offer both contraception and endometrial protection.
- Offer LNG-IUS insertion as part of preventive care when appropriate.
Hormonal IUDs and preventive care in Spanish clinics
Dr. Lucas and colleagues commonly offer LNG-IUS placement, follow-up visits, and non-operative management for selected precancerous conditions. Clinics in Spain may also provide bilingual counseling, fertility preservation discussions, and multidisciplinary coordination when needed.
Can Birth Control Be Used to Treat Precancerous Conditions?
Yes — in selected cases hormonal methods are therapeutic, not just preventive.
Endometrial hyperplasia explained
Endometrial hyperplasia is an overgrowth of the uterine lining that can precede cancer. Progestin therapy often reverses hyperplasia and is a cornerstone treatment for non-atypical and some atypical cases when fertility preservation is desired.
Fertility-preserving treatment options
For women who want to keep fertility, doctors like Dr. Lucas may recommend:
- High-dose progestin therapy (oral or LNG-IUS).
- Close monitoring with periodic endometrial sampling and ultrasound.
- Multidisciplinary planning involving fertility specialists if pregnancy is planned.
What Birth Control Does NOT Do?
While helpful, birth control is not an absolute shield.
Birth control is not a guarantee
Hormonal contraception lowers risk but does not eliminate it. Endometrial cancer can still occur — particularly if other strong risk factors are present.

Why screening and symptoms still matter?
Always report abnormal bleeding, pelvic pain, or new symptoms to your clinician. Regular gynecological follow-up remains essential, especially for women with risk factors or prior hyperplasia.
Risks and Side Effects of Hormonal Birth Control
Benefits must be balanced against potential harms, which vary by method and patient profile.
Blood clots, breast cancer, and myths
- Combined methods carry a small increased risk of venous thromboembolism (blood clots), especially in smokers and older women.
- Some studies show a small transient increase in breast cancer diagnosis among recent users; absolute risk is generally small and should be discussed with a doctor.
- Myths (e.g., birth control causes infertility) are not supported by evidence; fertility typically returns after stopping most methods.
When birth control may not be suitable?
Contraindications include a history of certain clotting disorders, uncontrolled hypertension, or recent major surgery with immobilization. Dr. Lucas evaluates personal health history before recommending options and offers non-hormonal alternatives when hormones are unsuitable.
Endometrial Cancer Prevention Beyond Birth Control
Birth control is one tool — a broader prevention plan matters.
Weight management
Maintaining a healthy weight reduces estrogen production from adipose tissue and lowers endometrial cancer risk.
Managing PCOS and diabetes
Treating underlying metabolic issues (PCOS, insulin resistance, diabetes) with lifestyle change and medical therapy reduces long-term risk.
Regular gynecological follow-ups
Routine care allows timely evaluation of abnormal bleeding, early detection of hyperplasia, and coordinated care for risk management. Dr. Lucas’ practice in Spain typically emphasizes combined medical, lifestyle, and procedural strategies tailored to each patient.
FAQs
Does taking the pill guarantee I won’t get endometrial cancer?
No. The pill reduces risk substantially but does not guarantee prevention. Continue regular follow-up and report any unusual bleeding.
Can my doctor use an IUD to treat early endometrial problems?
Yes. The levonorgestrel IUD is frequently used to treat endometrial hyperplasia and, in selected cases, as part of fertility-preserving therapy under close monitoring.
If I have PCOS, should I take birth control to lower cancer risk?
Many clinicians recommend progestin-containing contraception to regulate cycles and lower endometrial risk in women with PCOS, but the decision is individualized.
How do doctors in Spain approach this issue differently?
Spanish gynecologists often emphasize preventive counseling and may more commonly offer LNG-IUS as a dual contraceptive and therapeutic option; they also integrate lifestyle advice and multidisciplinary care.
What should I ask my doctor at my next appointment?
Ask about your individual endometrial cancer risk, which contraceptive options provide the best protective effect for you, side effects to expect, and monitoring plans if you have risk factors or precancerous changes.
Conclusion
Hormonal birth control that contains progestin — particularly combined oral contraceptives and the levonorgestrel IUD — reduces endometrial cancer risk in a meaningful way. For women in Spain and elsewhere, contraceptive choice should be individualized: weigh cancer-prevention benefits, side effect profiles, fertility goals, and personal risk factors with an experienced gynecologist. If you’re considering options, a consultation with a clinician such as Dr. Lucas can clarify the best strategy for both contraception and long-term uterine health.