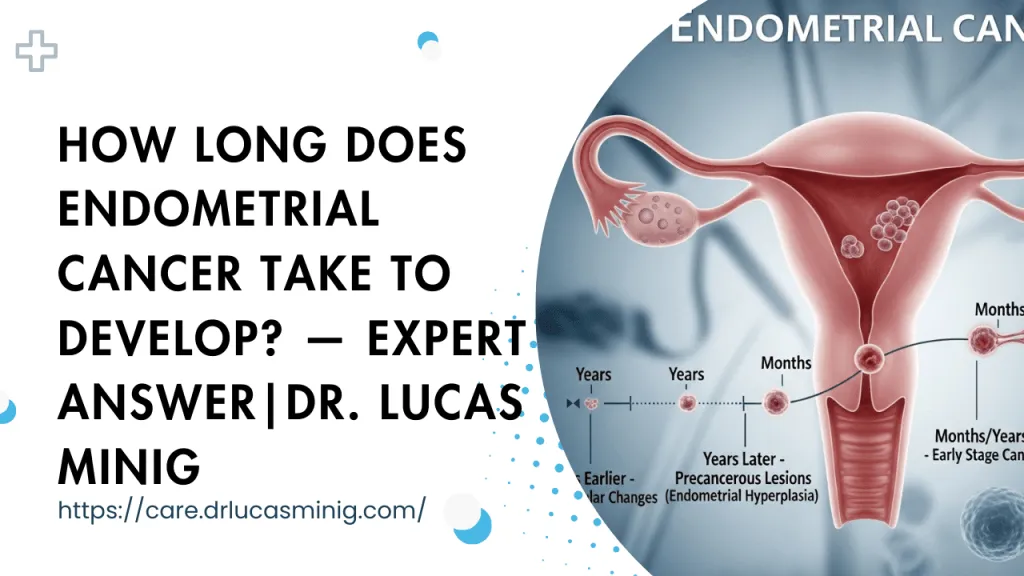
Discover the cause of endometrial cancer — unopposed estrogen, obesity, Lynch syndrome — and when to see a specialist. Expert care by Dr. Lucas Minig in Spain
Introduction
Endometrial cancer is a disease that begins in the lining of the uterus — the endometrium — and, like most cancers, develops when normal cellular controls fail. This page explains, in clear clinical language, the biological processes and common risk factors that lead to endometrial cancer, how clinicians in Spain and Europe investigate suspected causes, and what patients can do to reduce risk. Wherever relevant, I’ll reference how doctors such as Dr. Lucas Minig and other European specialists approach diagnosis, testing and prevention.
The Core Biological Cause of Endometrial Cancer
A clear and consistent biological explanation for many endometrial cancers is “unopposed estrogen.” In plain terms, when the growth-promoting effects of estrogen are not balanced by the stabilizing effects of progesterone, the endometrium is pushed toward continual proliferation. That repeated proliferation increases the opportunities for DNA mistakes, which can ultimately produce malignant transformation.
Uncontrolled cell growth explained simply
Imagine the endometrium as a garden. Estrogen is like fertilizer that encourages plants to sprout aggressively. Progesterone acts like the gardener, pruning and regulating growth. If fertilizer is applied constantly and pruning is absent, weeds (abnormal cells) can overrun the garden. Over time, some weeds develop characteristics that make them resistant to removal — that’s when a malignancy may form.
DNA mutations and cell repair
Every cell has mechanisms to repair DNA damage; when those repair systems work, mutations are corrected and the tissue remains healthy. When repair mechanisms fail — due to random errors, environmental exposures or inherited defects — mutations persist. Two concepts are important here:
- Somatic mutations accumulate with age and exposure to proliferative signals.
- Inherited defects (for example, deficiencies in mismatch repair genes seen in Lynch syndrome) reduce the ability to correct replication errors and markedly increase cancer risk.
When both high proliferative stimulus (unopposed estrogen) and inadequate DNA repair coexist, the probability of malignant transformation rises substantially.
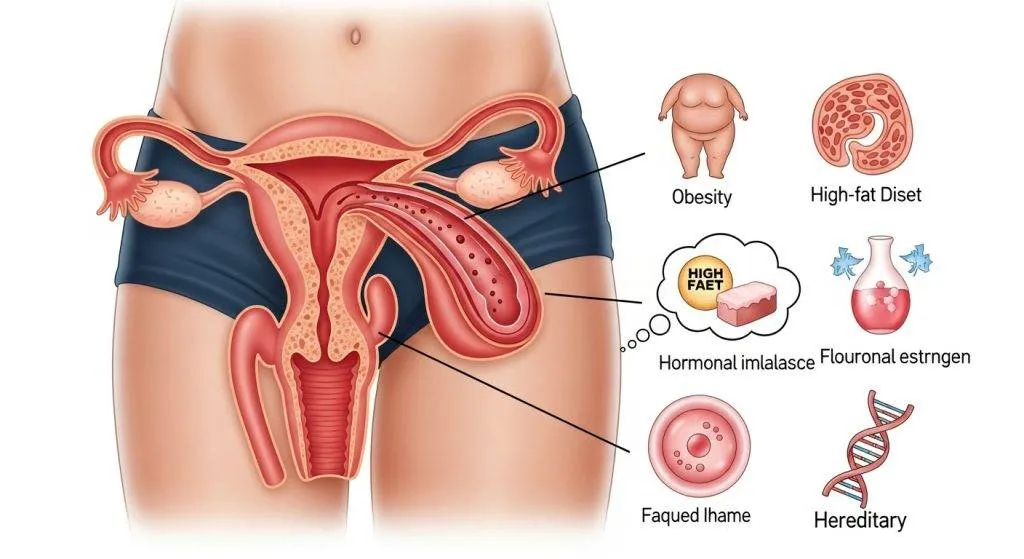
Major risk factors that explain the cause of endometrial cancer
Below are the principal causes and risk enhancers clinicians evaluate when determining why endometrial cancer has occurred.
Obesity and metabolic dysfunction
Obesity is one of the most important, modifiable contributors to endometrial cancer risk. Adipose tissue converts adrenal androgens into estrogen (a process called aromatization), increasing circulating estrogen levels — particularly in post-menopausal women. Obesity also causes insulin resistance and chronic inflammation, both of which promote cellular proliferation and can act together with hormonal effects to raise cancer risk.
Reproductive history: parity, menarche and menopause
Total lifetime exposure to menstrual cycles correlates with risk. Early menarche (early first period) and late menopause mean more years of cyclic endometrial proliferation. Conversely, pregnancies and breastfeeding suppress cycles for months to years, which lowers lifetime estrogen-driven growth and is therefore protective. Women who have never been pregnant (nulliparity) have a comparatively higher lifetime risk.
Chronic anovulation and PCOS
Polycystic ovary syndrome (PCOS) and other causes of chronic anovulation reduce progesterone exposure because ovulation (and the subsequent luteal phase) is the time when progesterone is produced. With fewer ovulatory cycles, the endometrium is often exposed to extended, unopposed estrogen — a condition that can lead to endometrial hyperplasia and, over time, cancer.
Hormone therapies and certain medications (tamoxifen, HRT)
- Tamoxifen is used for breast cancer prevention/treatment but acts as an estrogen agonist in the uterus in some patients, increasing the risk of endometrial pathology.
- Hormone replacement therapy (HRT): estrogen-only HRT in women with a uterus increases endometrial cancer risk; combining estrogen with a progestogen mitigates that risk. Prescribers in Spain and across Europe carefully tailor menopausal therapy to balance symptom control and oncologic safety.
Endometrial hyperplasia: the precursor lesion
Endometrial hyperplasia describes an abnormal thickening of the lining. When hyperplasia includes cellular atypia (abnormal cell appearance), the risk of progression to endometrial carcinoma is significantly higher. Detecting and treating hyperplasia — often with progestogen therapy or surgery depending on severity and patient goals — is a key prevention strategy.
Genetic causes: Lynch syndrome and family risk
A minority of endometrial cancers are linked to inherited mutations — most notably Lynch syndrome (defects in mismatch repair genes such as MLH1, MSH2, MSH6, PMS2). Women with Lynch syndrome face a substantially increased lifetime risk for endometrial (and colorectal) cancer. Identifying affected individuals enables targeted surveillance and risk-reduction measures for patients and relatives.
How do these causes differ by age and in post-menopausal women?
Endometrial cancer most commonly occurs after menopause, often presenting with post-menopausal bleeding. In post-menopausal women, obesity-driven estrogen and prior exposure history predominate as causes. Younger women who develop endometrial pathology typically have different contributing factors — PCOS, obesity, chronic anovulation, or genetic predisposition — and fertility preservation becomes an important clinical consideration. Clinicians adapt diagnostic and treatment strategies to age-specific priorities.

How doctors like Dr. Lucas Minig in Spain and Europe view and test for causes?
Clinicians practicing in major Spanish centers combine symptom-driven evaluation with risk stratification. Dr. Lucas Minig and colleagues emphasize rapid triage of abnormal bleeding, integrated use of imaging and tissue diagnosis, and early referral for genetic assessment when indicated.
Molecular testing and Lynch screening
- Tumor testing for mismatch-repair deficiency (IHC for MMR proteins or MSI testing) is commonly performed to screen for Lynch syndrome.
- When tumor testing suggests Lynch, germline genetic testing is recommended; this informs surveillance for patients and relatives.
Local practice: referral pathways and diagnostic ultrasound
- Typical pathway: primary evaluation → transvaginal ultrasound → endometrial biopsy (office or hysteroscopic) → pathology review → multidisciplinary discussion.
- In Spain, regional referral networks and specialized oncology units streamline care; a specialist such as Dr. Minig will often coordinate imaging, biopsy, and genetic consultation.
Symptoms that suggest the underlying cause may be progressing
The cardinal symptom that should prompt immediate evaluation is abnormal uterine bleeding — particularly bleeding after menopause or irregular/intermenstrual bleeding in pre-menopausal women. Other possible signs include persistent pelvic pain, unusual vaginal discharge, or systemic symptoms if disease is advanced. Because many underlying causes (for example, hyperplasia or Lynch syndrome) are silent until bleeding occurs, clinicians in Spain advise prompt assessment of any abnormal bleeding.
Prevention: addressing modifiable causes
Prevention aims to reduce the hormonal and metabolic environment that favours endometrial proliferation and malignant transformation.
Weight management and metabolic health
- Maintain a healthy BMI through diet, physical activity, and behavioral interventions.
- Treat insulin resistance and diabetes with lifestyle measures and medical therapy when required.
- Even modest weight loss can reduce peripheral estrogen production and inflammatory signaling.
Contraception, HRT choices, and ovulation regulation
- Combined oral contraceptives (estrogen + progestin) lower endometrial cancer risk when used long term.
- For menopausal symptoms in women with a uterus, combined HRT (adding progestin) mitigates the risk associated with estrogen-only therapy.
- For anovulatory patients, cyclic progestins or intrauterine progestin devices protect the endometrium and reduce hyperplasia risk.
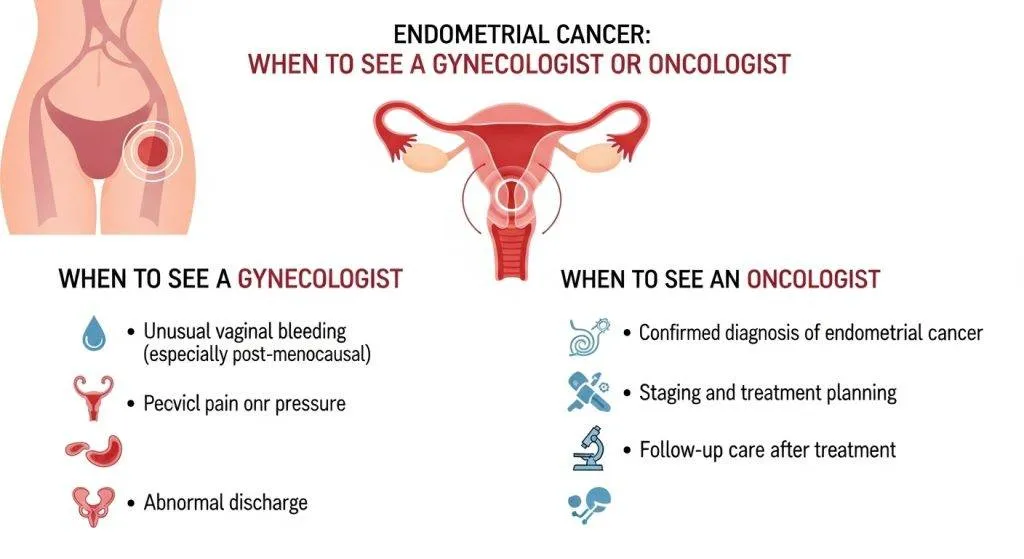
When to see a gynaecologist or oncologist?
Seek specialist evaluation if you experience:
- Any post-menopausal bleeding.
- New intermenstrual bleeding or persistent heavy periods.
- A known family history of Lynch syndrome or early colorectal/uterine cancers.
- Signs of metabolic syndrome plus irregular cycles (possible PCOS).
Specialists such as Dr. Lucas Minig can provide multidisciplinary assessment, surgical planning, and genetic counseling as needed.
Patient stories & the clinician perspective (doctor voice — Spain)
Clinicians in Spain often recount a common scenario: a post-menopausal woman presents with a small amount of bleeding, undergoes ultrasound and biopsy, and receives an early diagnosis followed by curative surgery. Doctors like Dr. Lucas Minig emphasize prevention (weight and metabolic control), prompt evaluation of bleeding, and consideration of fertility desires for younger patients — balancing evidence-based care with individual patient goals.
FAQs
What is the single biggest modifiable cause of endometrial cancer?
Obesity. Excess adipose tissue increases estrogen production and creates metabolic conditions that promote endometrial proliferation; losing weight reduces risk.
Can endometrial cancer be prevented?
While not all cases are preventable, many can be reduced by managing weight, controlling metabolic disease (diabetes), treating anovulation, and using appropriate HRT regimens. Regular evaluation for abnormal bleeding also prevents delayed diagnosis.
How is Lynch syndrome related to endometrial cancer?
Lynch syndrome is an inherited defect in DNA repair that markedly raises lifetime risk for endometrial (and colorectal) cancer. Identification leads to tailored surveillance and family counseling.
If I have abnormal uterine bleeding, what should I expect?
Expect a clinical history, pelvic ultrasound to assess endometrial thickness, and — if indicated — an endometrial biopsy or hysteroscopy to obtain tissue for diagnosis.
Do doctors in Spain follow different tests or standards?
Spanish clinicians follow European guidelines: they emphasize ultrasound and biopsy for abnormal bleeding, molecular testing (dMMR/MSI) to screen for Lynch, and multidisciplinary management. Local clinics often offer rapid-access evaluation pathways for symptomatic patients.
Conclusion
The cause of endometrial cancer is multifactorial but centers on a hormonal and molecular story: prolonged proliferative stimulation of the endometrium (most commonly unopposed estrogen) plus failures in DNA repair create the conditions for malignant change. Obesity, chronic anovulation (including PCOS), certain medications, endometrial hyperplasia and inherited syndromes (Lynch) are the main drivers. The good news: many risk factors are modifiable, and early detection — especially when post-menopausal bleeding occurs — greatly improves outcomes. If you have risk factors or symptoms, contact a gynaecologist or a clinic (for example, Dr. Lucas Minig’s practice in Spain) to arrange timely evaluation.