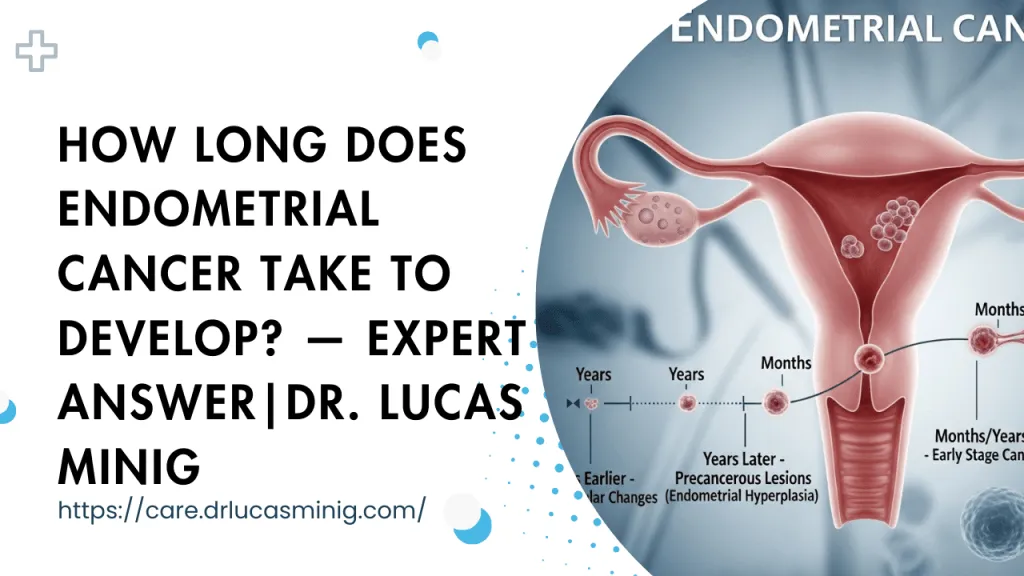
Not as rare as you think — discover Spain-specific numbers, warning signs, and fast steps to take. Expert guidance from Dr. Lucas Minig.
Introduction
Endometrial cancer — cancer of the uterine lining — raises a lot of questions: how common is it, who gets it, and should anyone worry? Below you’ll find a clear, evidence-based, and patient-friendly guide that explains global and Spain-specific numbers, lifetime risk, why many doctors don’t call it “rare,” and what to do if you or someone you love has symptoms. Where helpful, I’ll include practical notes about diagnosis and treatment in Spain.
How Rare Is Endometrial Cancer Worldwide?
Endometrial cancer sits among the more frequently diagnosed cancers in women globally — not as common as breast cancer, but far from rare.
Global Incidence Rates
Below are the headline global numbers that give scale to the problem:
In 2022 there were roughly 420,000 new cases of endometrial (womb) cancer worldwide, placing it among the top cancers affecting women globally.
These numbers show that endometrial cancer is a significant public-health issue, particularly in higher-income regions where it ranks higher among female cancers.
Latest global numbers
The most recent global cancer reports (GLOBOCAN and related sources) confirm rising absolute numbers of cases due to population ageing and increased prevalence of metabolic risk factors. This is why researchers and health systems track endometrial cancer trends closely.
Comparing endometrial cancer to other cancers
If you compare lifetime risk:
- Breast cancer remains the most frequent for women.
- Endometrial cancer is less common than breast cancer but more common than ovarian cancer in most developed countries.
- The practical takeaway: endometrial cancer is a common gynecologic malignancy and should be treated as a mainstream screening/diagnostic priority when symptoms arise.
How Common Is Endometrial Cancer in Spain?
Below you’ll find Spain-specific context — the most relevant part if you live in Spain or are researching local services.
Statistics and incidence rates in Spain
Recent Spanish cancer reports show that several thousand women are diagnosed with uterine (endometrial) cancer in Spain each year — numbers reported in the range of approximately 6,000–7,300 new cases annually, reflecting steady increases over the last decade. These figures underline that endometrial cancer is one of the leading gynecologic cancers in Spain.
Why cases are increasing in developed countries?
Developed countries show rising incidence because of an interplay of lifestyle and demographic changes.
The main reasons (in points for clarity):
- Rising obesity and insulin-resistance rates → more peripheral estrogen production.
- Aging populations → more women living into the decades of highest risk.
- Greater detection and diagnostic availability (ultrasound, endometrial biopsy).
- Changes in reproductive patterns (fewer pregnancies, later menopause in some groups).

Lifetime Risk: What Are the Chances of Getting It?
Understanding “how rare is endometrial cancer” requires separating annual incidence from lifetime risk.
Average lifetime risk for women
A practical way clinicians express risk: lifetime probability. For many populations the lifetime risk of endometrial cancer sits in the low single digits (roughly 2–3%, varying by country and population). That translates into a lifetime odds estimate commonly reported as about 1 in 35 to 1 in 50 women. While that’s lower than breast cancer risk, it’s still notable and justifies paying attention to symptoms and risk factors.
Risk by age group
Risk is very age-dependent: the risk rises with age and after menopause.
- Risk before menopause: Before menopause (under ~50), endometrial cancer is uncommon — it accounts for a small minority of cases (often quoted as <5%). Younger women generally have lower baseline risk unless they carry specific risk factors.
- Risk after menopause: After menopause the risk increases substantially. Most diagnoses occur in women aged 50 and older; that’s why postmenopausal bleeding is treated very seriously by clinicians.
Why Endometrial Cancer Is Considered “Not Rare” by Doctors
Doctors classify endometrial cancer as a common gynecologic malignancy — here’s why they say that.
Most common gynecologic cancer
Medical registries and clinical practice show that endometrial carcinoma outnumbers other uterine or ovarian tumors in many developed countries. It is therefore the most commonly encountered gynecologic cancer in routine oncology practice.
Why gynecologic oncologists see it frequently
- Many patients present early with bleeding or abnormal discharge (which prompts investigation).
- Surgical management (hysterectomy ± staging) is often indicated; gynecologic oncologists therefore see a steady flow of cases for operative care and follow-up.
- Advances in molecular profiling and minimally invasive surgery mean more patients are referred to specialized centers for tailored management.
Who Is Most Likely to Develop Endometrial Cancer?
The risk profile is well described and includes both modifiable and inherited risks.
Age and menopause
Most cases are post-menopausal — the single biggest demographic risk factor is increasing age. Women in their 60s and 70s represent a large share of diagnoses.
Obesity and hormonal factors
A few lines before point list: obesity and hormonal exposure are central drivers — and this is an area where prevention efforts can help.
- Excess body fat increases estrogen levels without the balancing effect of progesterone.
- Long periods of unopposed estrogen exposure (e.g., certain hormone treatments or anovulatory cycles) raise risk.
- Diabetes and metabolic syndrome are strongly linked as well.
Genetic risk factors
A smaller proportion of cases are related to inherited syndromes: for example, Lynch syndrome (hereditary nonpolyposis colorectal cancer) substantially increases lifetime endometrial cancer risk. For women with a strong family history of colorectal or endometrial cancer, genetic counseling is recommended.
Rare Subtypes vs. Common Types
Intro line: “endometrial cancer” is an umbrella term — most cases are one kind, while a few subtypes are uncommon but important.
Endometrioid Carcinoma (Most Common Type)
Brief lead: the bulk of endometrial cancers belong to the endometrioid histologic type — the “garden variety” that tends to be hormonally driven and often has a better prognosis. Endometrioid tumors account for roughly 85–90% of diagnosed cases in many series.
Uterine Serous Carcinoma and Other Aggressive Forms
Short intro: a smaller proportion of cases are aggressive histologies that behave more like ovarian cancer.
- Serous and clear-cell carcinomas are less common but have higher recurrence risk and worse prognosis.
- These forms often require more aggressive multimodality therapy and specialist input.
Uterine Sarcoma – A Truly Rare Entity
A one-line note: uterine sarcomas arise from muscle or connective tissue and are biologically distinct — they are rare compared with endometrioid carcinomas and are managed differently by gynecologic oncology teams.
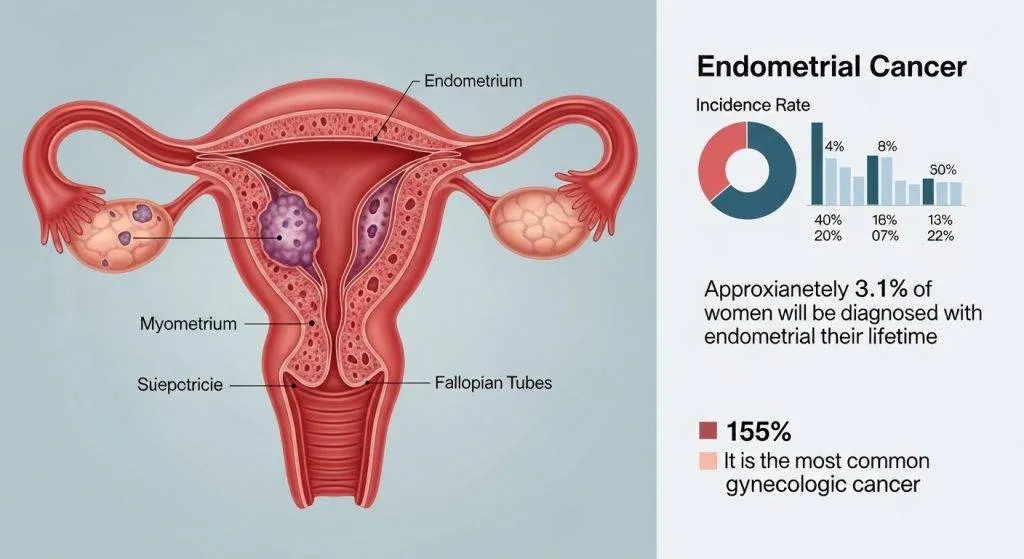
Signs and symptoms: when to see a doctor
Symptoms usually prompt evaluation, which is why many cases are caught early.
Red flags: post-menopausal bleeding
The single most important alarm signal is vaginal bleeding after menopause. Studies and guideline reviews find that the vast majority of women with endometrial cancer report bleeding as the presenting symptom — roughly nine out of ten of diagnosed cases — so any postmenopausal bleeding should prompt urgent evaluation.
Other symptoms that matter
If you have any of these, see your doctor:
- Abnormal bleeding between periods (for premenopausal women).
- Persistent pelvic pain or pressure.
- Unusual watery or blood-tinged vaginal discharge.
Early evaluation improves outcomes.
Diagnosis — what to expect in Spain (tests & pathway)
Spain’s health services have clear pathways from primary care to specialist gynaecology/oncology.
Primary care → specialist referral
In Spain the diagnostic pathway commonly begins with a primary-care or gynecology visit. A clinician will take a history, perform a pelvic exam, and arrange a transvaginal ultrasound or direct endometrial sampling, depending on the situation. If imaging or sampling suggests malignancy, referral to a gynecologic oncology team follows.
Typical tests (ultrasound, biopsy, MRI)
Before the specifics: the diagnostic workup is stepwise and focused on confirming diagnosis and staging.
- Transvaginal ultrasound (TVUS): measures endometrial thickness and helps decide if biopsy is needed.
- Endometrial biopsy or curettage: definitive tissue diagnosis.
- Pelvic MRI / CT: used for local staging and planning surgery when cancer is confirmed.
This pathway is common in Spanish public and private centers; efficient coordination reduces delay to treatment.
Treatment overview & outcomes
Treatment depends on stage and histology — many cases are curable.
Early-stage prognosis
When detected early, surgery (usually hysterectomy with staging) can be curative. Minimally invasive approaches (laparoscopy or robotic surgery) are often used, reducing recovery time and complications. Many patients have excellent 5-year survival when the disease is confined to the uterus.
Advanced disease: options & hope
For regional or advanced disease, treatment becomes multimodal — surgery, radiation treatment, chemotherapy and, increasingly, targeted or immunotherapy options guided by molecular profiling. Though outcomes are poorer than for early disease, ongoing research is expanding treatment choices and survival is improving for selected patients.

Expert Perspective: Dr. Lucas Minig on Endometrial Cancer in Spain
A practicing gynecologic oncologist’s viewpoint helps translate data into patient action.
Why Specialized Surgical Care Matters
Dr. Minig emphasizes that accurate intraoperative assessment and tailored surgery are crucial. For many women in Spain, early-stage disease means less radical surgery and faster recovery — but complex or aggressive cases need referral to a gynecologic oncology center where experienced surgeons and multidisciplinary teams collaborate.
Minimally Invasive Treatment Approaches
Dr. Minig and his colleagues in Spain increasingly favor minimally invasive and robotic techniques when oncologically safe, since these approaches often reduce hospital stay and speed functional recovery — a major quality-of-life consideration for older patients or those with comorbidities.
Conclusion
Endometrial cancer is not rare — globally or in Spain — and it represents a common, well-recognized diagnosis with clear red flags (especially post-menopausal bleeding), known risk factors, and strong prospects for cure when detected early. Public-health trends (aging populations and rising obesity) mean case numbers are rising in developed countries, which makes prevention, awareness, and timely specialist referral more important than ever. If you’re in Spain and have concerning symptoms, reach out to your GP or a specialist like Dr. Lucas Minig for prompt evaluation.
FAQs
Is endometrial cancer rare in women under 40?
Yes — it’s uncommon before menopause (<5% of cases), but young women with risk factors (PCOS, obesity, Lynch syndrome) should remain vigilant.
How often does endometrial cancer present with bleeding?
The majority of cases (~90%) present with vaginal bleeding, particularly postmenopausal bleeding, which is why that symptom triggers rapid evaluation.
What is the best way to check for endometrial cancer?
A transvaginal ultrasound followed by endometrial biopsy (if indicated) is a standard diagnostic pathway; MRI is used for staging after a diagnosis.
Can lifestyle changes reduce my risk?
Yes — maintaining a healthy weight, controlling diabetes and avoiding unopposed estrogen therapy where not needed all lower risk.
What are survival chances if cancer is found early?
Very good — localized disease has high 5-year survival rates (often above 80–90% in many registries), which is why early diagnosis is so important.